Synvisc, also called hyaluric acid, is injectable medication used in the treatment of osteoarthritis.
Hyaluric acid is an important component of articulat cartilage. It binds water and is responsible for the resilience of cartilage. Osteoarthritis, unfortunately erodes the articular cartilage of a joint giving rise to pain and reduction in range of motion.
Synvisc when injected into a joint is commonly referred to as viscosupplementation. It is thought that Synvisc supplements the viscosity of the joint fluid thereby lubricating the joint whereby in theory reducing the level of pain.
It can be injected in the knee, hip and shoulder joint.
The manner in which it is injected is critical. Most clinician inject the joint without x-ray guidance which can result in the deposition of the Symvisc outside of the intended joint. This can and often times does create a significant amount of pain and affords the patient no therapeutic response since the medication was not delivered into the intended joint. Jackson demonstrated that experienced orthopedics physicians are only successfully in entering the knee joint space 71% of the time when using an anterolateral approach WITHOUT x-ray. At the Centeno-Schultz Clinic x-ray is always utilized with viscosupplementation to ensure accurate placement of the medication and to avoid the pain associated with injection of hyaluric acid outside of the joint space.
If Snyvisc therapy fails to provide significant pain relief, patients now have the option of utilizing their own meseenchymal stem cells to regenerate cartilage in the knee, hip and shoulder. It is a novel, needle-in, needle-out procedure with allows patients to avoid the risk of disease transmission as well as the trauma and rehabilitation associated with surgery.
Please review knee MRI below of patient who underwent the use of her own mesenchymal stem cells to regenerate cartilage. Pre-treatment images are on the top and demonstrate a cartilage depth ranging between 0.2- 0.3cm. Five months post therapy, the cartiage has increased on average by 1mm.

Regeneration of knee cartilage through stem cell therapy
Clinically the patient has had a significant reduction in her pain and an increase in her range of motion. We just received an e-mail from her along with a picture of her daily activity:)

Back to Loving Life
synvicinectionpain.synaviscinjectionpain.muscleatrophyinoneshoulder.physcialtherapyaftershouldersurgery.





 Tendons are fibrous connective tissue that attach a muscle to bone.
Tendons are fibrous connective tissue that attach a muscle to bone.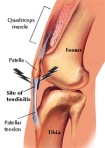







 Often times surgery is the recommended therapy.
Often times surgery is the recommended therapy.





